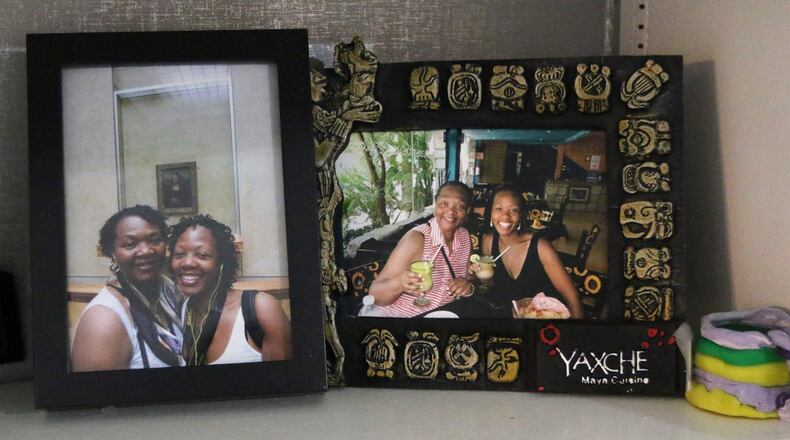I was packing a suitcase in metro Atlanta with my daughter, Dr. Shalon Irving, three weeks after she gave birth to my granddaughter, Soleil.
This wasn’t just any weekend trip. It was the mother-daughter getaway Shalon had planned and saved for, a way of introducing Soleil to the thing she loved almost as much as science: Seeing the world.
She did “everything right.” She was a Centers for Disease Control and Prevention (CDC) epidemiologist. She knew the risks of Black maternal mortality and postpartum hypertension better than most of the clinicians who would treat her.
She chose a strong OB-GYN, built a detailed birth plan and followed every instruction to bring Soleil into this world safely.
And yet, Shalon had been trying to tell providers she didn’t feel right after childbirth. Her blood pressure was dangerously high. Her legs were swollen. She was gaining weight rapidly. And still, they sent her home.
That night, as we packed, my daughter collapsed. She would never wake up. Shalon died just seven days later from childbirth-associated blood pressure complications.
Ga. gets an ‘F’ on maternal mortality rate
Credit: Handout
Credit: Handout
Shalon was so much more than a maternal mortality statistic. She served as a lieutenant commander in the U.S. Public Health Service Commissioned Corps. She was the first student to earn a dual-titled Ph.D. in sociology and gerontology from Purdue. She was committed to putting research into practice, working with communities and using participatory approaches that treated people as partners, not simply subjects. She was a once-in-a-generation public health mind.
And yet, the system that is supposed to keep new mothers alive failed her anyway.
Georgia’s maternal health crisis isn’t new. The March of Dimes recently gave Georgia a failing “F” grade, and the state’s maternal mortality rate remains among the nation’s highest at 37.9 deaths per 100,000 live births, and 87% of cases are deemed preventable.
Of course, this isn’t only about Georgia. Nationally, the CDC reports the maternal mortality rate for Black women was more than triple the rate for white women.
My heart broke all over again reading about the recent death of Dr. Janell Green Smith - a 31-year-old South Carolina midwife and outspoken Black maternal health advocate who died from childbirth complications.
If women with the expertise, credentials, and persistence that Dr. Green Smith and my daughter had couldn’t get lifesaving care, what chance does any mother have?
We need investment and accountability on maternal health
It’s been nine years since we lost Shalon. And too much has stayed the same. I’m tired of reliving the tragedy of my daughter every time I read a headline about another Black mother lost to a system built to discount their pain.
And yet, just when we should be strengthening the safety net, the federal infrastructure that is meant to prevent maternal deaths is under threat.
The federal government helps states track maternal deaths, study patterns and put real prevention measures in place — the kind of work that could have raised red flags sooner, trained providers better and saved lives. But a sweeping restructuring at the Department of Health and Human Services has put that infrastructure at risk, and a coalition of states has sued over it.
I recently joined an amicus brief alongside other families and community-based groups in that lawsuit because it is one way families like mine can speak directly to the court—not as lawyers or politicians, but as people living with the consequences.
Credit: Emily Haney
Credit: Emily Haney
My daughter believed in public health because she believed our government could do better - if we demanded it. Gutting the very programs designed to understand maternal deaths and prevent them doesn’t make Georgia safer. It makes it easier to look away.
I’m using my voice now because Shalon isn’t here to use hers. Her personal and professional mantra was so simple and so fierce: “I see inequity wherever it exists. I am not afraid to call it by name and work hard to eliminate it. I vow to create a better earth.”
I hope our story inspires more Georgians to use their voices, too — to call state legislators and demand real investment, transparency, and accountability on maternal health.
To insist on care standards that treat postpartum hypertension as the emergency it is. And to support community-rooted maternal health organizations, like 4Kira4Moms and the one we created in Shalon’s memory.
Soleil will know who her mother was — not just in photos and memories we share, but in the research she left behind and the change we’re still fighting for. She deserves to grow up in a Georgia where new motherhood isn’t life-threatening and where Black women are believed in time to be saved.
Wanda Irving is the founder, CEO and board chair of Dr. Shalon’s Maternal Action Project.
About the Author
Keep Reading
The Latest
Featured